Iron lung and other respirators
The iron lung was invented in 1929 by Philip Drinker (1893-1977), a professor at the School of Public Health at Harvard University. The device performs the function of the muscles that control breathing. It was one of the first of several inventions designed to keep people alive who are unable to breathe unassisted.
Pulmonators
During the 1920s people who could not breathe on their own were aided by a pulmotor. This was a machine similar to fireplace bellows. It inflated and deflated the lungs by forcing air in and then sucking it back out again. The process worked, but some patients experienced chest pain. Many people suffering from polio or infantile paralysis required such a device. The polio virus can damage the nervous system causing paralysis of the diaphragm. Without the movement of the diaphragm, polio-sufferers often died by suffocation.
Drinker's Research
Drinker got his idea from a Swedish physician named Thunberg, who had been experimenting with a vacuum device to help patients breathe. Drinker enlisted the help of his brother, Cecil, and Louis Shaw (1886-1940) to build a prototype (model) based on Thunberg's principles. He tested the first machine on cats and then designed one large enough for a human patient.
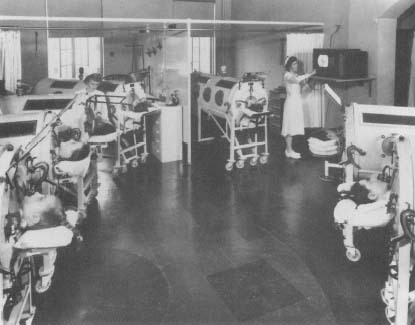
The patient's head was positioned outside the box while the rest of the body was enclosed in the airtight metal box. A pump connected to the box varied the air pressure inside the chamber. When the air pressure inside the box decreased, the weight of the atmosphere outside the box forced air through the nose and mouth into the lungs. When the air pressure in the box increased, the air was forced out of the lungs.
Drinker's invention was first known as the "Drinker tank respirator" but was soon given the nickname of "iron lung." Drinker and Louis Shaw received numerous awards for their invention. The iron lung allowed many polio patients to live longer lives. It was used from 1928 well into the 1950s.
Ventilators
Since Drinker's time, a sophisticated class of breathing machines called ventilators, or respirators, has been developed. A modern ventilator consists of an electrical pump connected to an air supply, a humidifier that adds water to the air, and a tube inserted into the patient's nose or mouth. Ventilators use positive air pressure from the pump to force air into the lungs. The ventilator pumps air into the lungs for a preset time or volume and then stops. The patient then exhales the air naturally.
To adjust the ventilator properly, a blood sample from the patient is analyzed. This determines the metabolic rate and the optimal oxygen-carbon dioxide ratio. Then the volume of air needed and the number of times per minute the person should breathe to maintain the desired metabolic rate
Ventilators aid patients who have paralyzed muscles, suffer from degenerative muscle disease, or have burns in the nose and throat. When patients are to be hooked up to a ventilator for months at a time a breathing tube is surgically inserted directly into the windpipe. Miniature ventilators are used to help premature babies breathe. They are also used to help patients who have undergone surgery and need temporary help from a machine.
In some places, the iron lung of the 1950s is making a comeback. Because it uses non-invasive technology and negative air pressure (a vacuum), it does not cause infections or scarring of the trachea. It can be used at home to help a patient rest the respiratory muscles during the day or night.
Mini-iron lungs are now used for some patients. Nicknamed "turtles" because of their green color and shell-like shape, these miniature devices can be strapped onto a patient's chest.
Thanks,
Lilly
In theory a device could perform this by using an air tight seal to suck away the air from the belly so the normal air pressure outside the person will be forced into the lungs exactly like the original iron lung has faithfully done.
regards Terry
sure,going into the "tank" is traumatic but compared w/being "tubed" ?
no contest.
in certain situations it definitely should be used and revived for use.
to those enquiring and concerned about inability to find part ? they're still out here and gawdforbid, with the internet,replacement cn either be found or made-
the one looking for mobility--investigate the cuirass
these items are STILL USED and have their own proven track record.